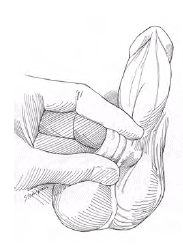
No-Scalpel Vasectomy
A Minimally Invasive Form of Permanent Birth Control

If your family is complete and you are looking for a practical, permanent form of birth control, vasectomy offers real advantages over other methods.
The surgery is now simpler, shorter and less painful than ever. After a quick, in-office procedure and a day or so of recovery, you can enjoy the freedom and spontaneity of no longer worrying about contraception.
Selecting a skilled provider can put your mind at ease about the procedure. Dr. Paul Turek is an internationally renowned expert in men’s sexual health, and is frequently sought after for his world-class surgical expertise. He will educate you about your treatment options, answer all your questions and help you understand what to expect. Dr. Turek’s warm, affable style will put you at ease and create a comfortable learning environment.
Expertise You Can Trust
Men come from all over the world to see Dr. Turek, a fellowship-trained microsurgeon who has performed well over 2,500 no-scalpel vasectomy procedures. Dr. Turek has been named one of the “Best Doctors in America” by no fewer than seven accrediting agencies, and he has helped to train more than 60 doctors, residents and fellows in the no-scalpel vasectomy procedure.
Procedural Details, Step by Step
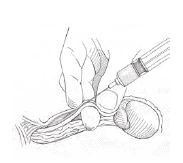
The modern vasectomy procedure is simple, short and very effective at preventing pregnancy. It is designed to interrupt the normal flow of sperm by closing off the vas deferens, the tubes that transport sperm. After the procedure, the testicles continue to produce sperm, but the sperm don’t enter the ejaculate. And you won’t notice a change in the amount of semen either.
During your initial consultation with Dr. Turek, he will discuss the procedural steps using simple, comprehensible language and illustrations so you understand exactly what it involves.
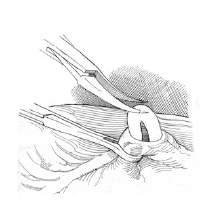
The Single Most Effective Form of Contraception
Vasectomy has the highest success rate out of any type of birth control currently available. In other words, there is no more effective contraception available anywhere. If you do not want to worry about contraception, vasectomy offers complete peace of mind with no adverse effects on sex drive, erections or ejaculation.
Repairing Failed Vasectomies
Although vasectomy is the most effective way to prevent pregnancy, it is not perfect. Vasectomies can fail if performed by an unskilled or inexperienced doctor or if the post-operative instructions regarding protected intercourse are not followed. Because of his global reputation as a trusted men’s health provider, Dr. Turek is often referred cases of failed vasectomies performed elsewhere.
Dr. Turek’s Minimally Invasive, Minimal Touch Technique
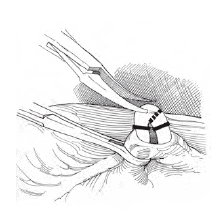
Dr. Turek’s preferred surgical method is the no-scalpel vasectomy, which involves no incisions. Another technique, called the no-needle vasectomy, involves delivering anesthesia via a compressed air device (or “spray gun”) instead of through a needle. However, the spray gun emits a loud noise that is often startling for patients.
To avoid both the sting of the needle and the disconcerting noise of the spray gun, Dr. Turek prefers an alternative “minimal touch” technique, which allows him to quietly numb the area while you remain calm, relaxed and comfortable. Uniquely, by performing an “in-line” procedure and by not removing any tissue for any reason, he puts everything back the way it was found.
Low Risk of Complications

Vasectomy is also one of the safest forms of permanent birth control; however, as with any surgery, there are risks to carefully consider. Dr. Turek will discuss his carefully tracked, individual experience with these risks and address your questions and concerns, so you have the information you need to make decisions about your care.
Frequently Asked Questions About No-Scalpel Vasectomy
What is a vasectomy?
A vasectomy is a form of permanent birth control that “disconnects” the vas deferens, the tube that carries sperm from the testicles to the ejaculate.
Is a vasectomy effective at preventing pregnancy?
Vasectomy is the single most effective form of contraception. It is quick, minimally invasive and has a very low complication rate when performed by someone as experienced as Dr. Turek.
How does a vasectomy compare to contraceptive methods for women?
Contraceptive methods for women such as the oral pill or intrauterine devices are far from ideal. Not only can many methods fail, they are not always well-tolerated and can have unpleasant side effects. Vasectomy is safe, reliable and hormone-free.
What is a no-scalpel vasectomy?
A no-scalpel vasectomy is performed through a tiny opening in the scrotal skin. There is no cut, only a small puncture. The skin is spread and the vas deferens is brought to the skin and cut, cauterized and clipped. Then, the vas deferens is placed back in the hole, which closes up on its own.
Is a no-scalpel vasectomy painful?
No-scalpel vasectomy is not a painful procedure. Dr. Turek understands pain is probably one of your foremost concerns when considering a vasectomy, and he provides the highest level of care to prevent pain during and after the procedure. (Think of it as a very quick dentist office visit.)
How long does it take to recover from a vasectomy?
Most patients are able to return to work one to two days after a vasectomy. Mild aftereffects include light spotting and swelling, which usually subside within 72 hours of the procedure. You will be advised to avoid strenuous exercise and heavy lifting for four days and to refrain from sex for seven days.
How long does a vasectomy take?
Vasectomy is a fairly quick outpatient procedure and can usually be completed in approximately 30 minutes of your time from entering until leaving the office.
What are the risks of vasectomy?
Very rarely (<0.1 percent) hematomas, or clots of blood, can form in the scrotum. Small blood clots can be reabsorbed by the body over time, but large clots may require a surgical procedure to treat.
Another risk is that the vasectomy fails and leads to sperm in the ejaculate and pregnancy. Dr. Turek’s vasectomy failure rate is incredibly low, with less than 1 in 2,000 cases failing.
Men worry most about pain after vasectomy. In Dr. Turek’s experience, men take an average of two pills of some kind after his procedure. He has no patients with chronic pain, which is estimated to occur in 15 percent of all men getting vasectomies.
Do I need to be put under anesthesia for a vasectomy?
No, you will be awake during the procedure. The treated area is completely numbed with local anesthesia ointment and injection, so you will not feel any pain.
Can I have sex right after healing from a vasectomy?
You can have sex after you have healed from your vasectomy, but you should use another form of protection to prevent pregnancy until your semen has been tested to prove no more sperm are present. Sperm can survive for several months in the vas deferens above the point where the tube was interrupted. It can take 30 ejaculations to completely empty the vas deferens of sperm. Dr. Turek will ask you to provide a semen sample approximately three months after vasectomy; at this point, 90 percent of men have no sperm in their ejaculate.
Talk to Our Internationally Renowned Men’s Health Expert
If you would like to put your worries about an unplanned pregnancy to rest, vasectomy offers many advantages over other birth control methods. To learn more about the no-scalpel vasectomy from a trusted men’s health provider, please request a consultation with Dr. Paul Turek by calling or emailing The Turek Clinic today.