In Vitro Fertilization vs. Intracytoplasmic Sperm Injection
In vitro fertilization or IVF has been around for over 40 years and is a proven treatment for many forms of female and male infertility. It has even earned itself a Nobel Prize. Known as “test tube baby” technology, it is more aptly called “petri dish conception.” By putting half a million sperm and one egg really close together in a dish, it facilitates the egg fertilization process that might not otherwise occur. And although there is no “was-it as-good-for-you-as-it-was-for-me” moment with IVF, it still allows for God or Darwin to select the best sperm for the egg, retaining the essence of natural selection and organic evolution.
Is More Better?
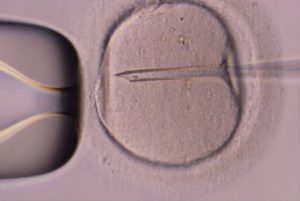
Intracytoplasmic sperm injection or ICSI, on the other hand, is a natural-selection-altering “add on” technique used with IVF. Developed somewhat by chance in Belgium in 1992, it allows for effective egg fertilization by the injection of a single sperm into a single egg. Although this has opened up the possibility of fatherhood for men with very low sperm counts and men with no ejaculated sperm (but with testicular sperm), by its very nature, it alters natural selection. This is because the sperm placed in the egg is chosen by a hard-working, but ultimately human, embryologist, based on how that sperm looks and moves. And there’s no evidence that even the best human being has any idea what God or Darwin is thinking in selecting the “chosen” sperm. Given this, we need to ask ourselves exactly how ICSI might be altering human development and evolution. Indeed, Dr. Carl Djerassi, inventor of the birth control pill, was so impressed with the way ICSI altered his view of conception that he penned a famous play called “An Immaculate Misconception.”
At its birth, ICSI was used solely for men with low sperm counts or men who needed surgical sperm retrieval. Then, it became popular for those with plenty of sperm but whose sperm shape was abnormal. Then the big creep began: Over the last 20 years, its use case has now expanded to include female factors such as reduced egg number or maturity, frozen-thawed eggs, and now just “unexplained” infertility. Currently the “go-to” procedure in the world of assisted reproduction, ICSI was used in 155,647 U.S. IVF cycles in 2017, a whopping 63% of all cases. As a procedure that increases the cost of IVF by $1-2K, the million-dollar question about ICSI is whether its widespread use is really justified.
Less is More
Well, two studies have now robustly answered this question. The first was published in 2001 and performed in the U.K. It reported the success rates among 435 infertile couples who were randomized to either IVF or IVF-ICSI for fertility treatment. Importantly, none of the couples had male factor infertility, which is the original indication for using ICSI. The question the research answered in a randomized clinical trial (the most powerful study design ever conceived) is whether ICSI would improve pregnancy outcomes when used strictly for female factor infertility. The answer was clear: IVF led to higher pregnancy rates (by almost 20%) than ICSI did when used to treat female infertility. The first sign that more technology may not be better.
The second robust study on this topic was published this year (2021). This research was also a randomized clinical trial, but a much larger one (n=1064 couples). Importantly, it examined the most relevant fertility endpoint: live births. Couples with normal sperm counts and motilities (i.e. no male factor infertility) were again randomized to either IVF or IVF-ICSI. And lo and behold, couples in both groups were equally likely to have a baby. Even more evidence that less is more.
In summary, ICSI was developed to treat severe male factor infertility. And it does this with aplomb. But now, it’s used to treat virtually all forms of infertility and without good reason. And the best data now confirms that ICSI does not improve the chances of having a baby when compared to IVF in the vast majority of scenarios in which it is used. In the words of Oscar Wilde: “We live in an age when unnecessary things are our…necessities.” Given the unknowns surrounding ICSI and its potential to alter human development and evolution, it is perfectly reasonable to just say “No, thank you!”









